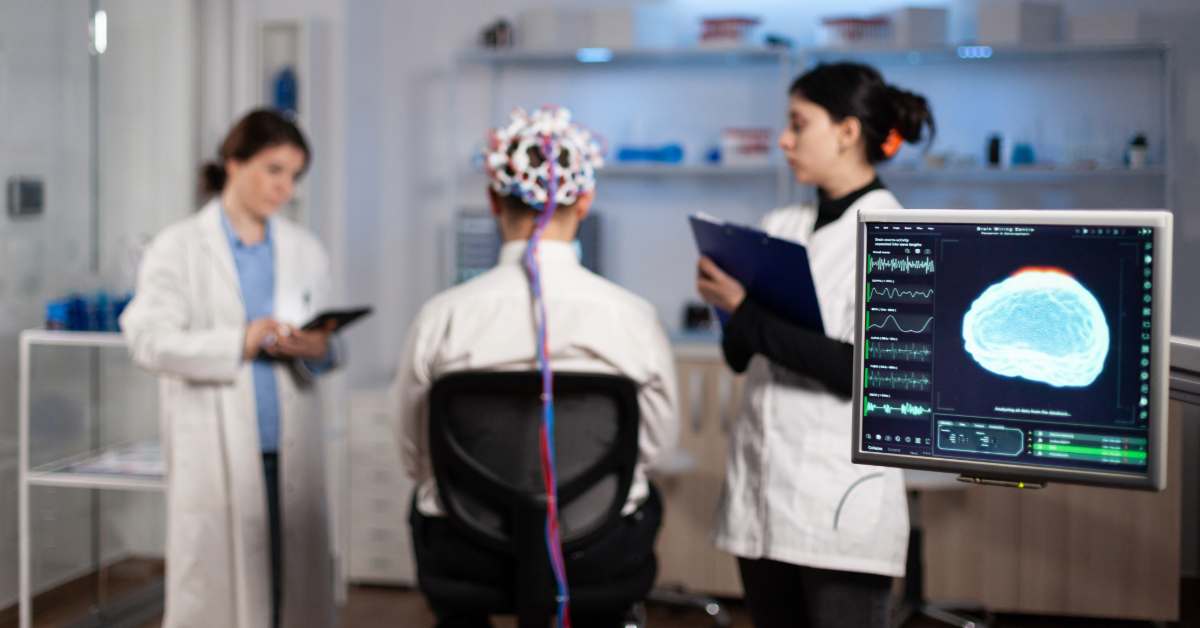
New research shows that patients with cancer in Denmark undergoing colorectal surgery face significantly fewer complications and hospital readmissions when an artificial intelligence tool is used to support treatment planning.
AI Significantly Lowers Risks for Colorectal Cancer Patients
A newly published study reveals that post-surgery recovery for patients with colorectal cancer in Denmark improves markedly when treatment plans are guided by artificial intelligence (AI). Developed by researchers from Zealand University Hospital and the University of Copenhagen, the AI tool has proven to reduce medical complications after surgery by as much as 36% and decrease hospital readmissions by 35%. The results show AI can help patients heal better.
Save money on Electricity...
See the cheapest electricity prices in Denmark and save money.
The groundbreaking study, recently published in the prestigious journal Nature Medicine, documents how AI can be successfully integrated into clinical settings to make surgeries and recovery more personalized and efficient. The AI tool tailors treatment before and after surgery, considering factors like prehabilitation, nutritional needs, and follow-up care. Many people will recover faster.
Customized Treatment Before and After Surgery
The innovative AI system was created using a vast reservoir of Danish health register data. It predicts a patient’s likelihood of survival within a year of undergoing colorectal cancer surgery, and recommends treatment adjustments accordingly. The model has been tested on a group of 1,000 patients from Zealand University Hospital.
These patients were placed into risk-stratified categories, allowing doctors to adjust their care plans based on individual needs. Measures include customized physical training and dietary support, inspired by strategies from the international PREHAB initiative, which promotes proactive healthcare interventions prior to surgery for cancer in Denmark.
High-Risk Patients See Greatest Benefit
The most encouraging findings from the study center on patients with the highest risk profiles. Among this group, the AI-assisted approach yielded the most substantial reductions in post-surgical complications and rehospitalizations, suggesting the tool is especially effective for the most vulnerable populations.
This is particularly significant considering that complications following colorectal surgery can often lead to prolonged recovery, secondary illnesses, and substantial emotional and financial burdens for patients and the healthcare system.
Substantial Cost Savings for Healthcare System
Beyond enhancing clinical outcomes, the study also highlights economic benefits. The use of the AI system is linked to a reduction in demand for healthcare services following surgery. Researchers estimate that the tool could free up approximately 18,000 Danish kroner (equivalent to around $2,600 USD) per patient by reducing the need for further care.
Save money on Electricity...
See the cheapest electricity prices in Denmark and save money.
With thousands of colorectal surgeries performed each year in Denmark alone, the potential cost savings for hospitals and public health systems could reach into the millions. These promising numbers strengthen the case for integrating AI tools not only in cancer care but more broadly across medical fields.
Expanding the Scope Beyond Colorectal Cancer
Building on these results, the research teams now plan to explore how AI can be implemented to enhance care for patients with other types of cancer in Denmark, including lung, kidney, bladder, and ovarian cancer. The goal is to continue developing decision-support tools that fit seamlessly into everyday clinical practice, delivering improved outcomes for a wider range of patients.
Unlike many algorithmic tools that remain in the development stage or are confined to academic research, this AI model has already undergone real-life application, marking a crucial step towards the digital transformation of health services in Denmark and beyond.
Data-Driven Medicine in Denmark
This project is an example of how Denmark continues to lead the way in digital health innovation, taking advantage of its highly organized and centralized healthcare data systems. The country’s comprehensive patient records have allowed researchers and healthcare providers to collaborate effectively, resulting in tools that are informed by real clinical patterns and outcomes.
As other countries look to modernize their healthcare systems, the Danish model demonstrates the value of combining AI technologies with structured national health data to deliver safer, more efficient, and more cost-effective treatment. With these findings now published internationally, broader adoption of AI healthcare tools may be closer than ever.